High blood pressure is often framed like a personal failure. Eat better, move more, sleep well, take the pills. But a newer explanation is pushing that story in a more useful direction. Hypertension can become a self-feeding problem inside the blood vessels themselves.
The scale is hard to ignore. Official global estimates show that in 2024, about 1.4 billion adults ages 30 to 79 had hypertension, and only about 320 million had it under control. About 600 million did not even know they had the condition.
Not just poor habits
Fernanda Montes de Oca, a clinical physician with training in nutrition science and advanced immunology, puts the issue bluntly. “Blood pressure does not get worse only because the patient ‘does not take care of themselves.’ It gets worse because it is a disease that, once started, changes the structure of the system that regulates it,” she said in comments reported in March 2026.
That does not mean habits do not matter. Smoking, excess weight, stress, poor sleep, and too much sodium can still push blood pressure up. The point is more subtle. Once the system is under strain, the body may start protecting blood flow in ways that keep pressure high.
What pressure measures
Blood pressure is the force of blood pushing against artery walls as the heart pumps. A U.S. federal health resource also notes that high blood pressure usually has no symptoms, which is why regular checks matter. Left untreated, it can raise the risk of heart attack, stroke, heart failure, and kidney failure.
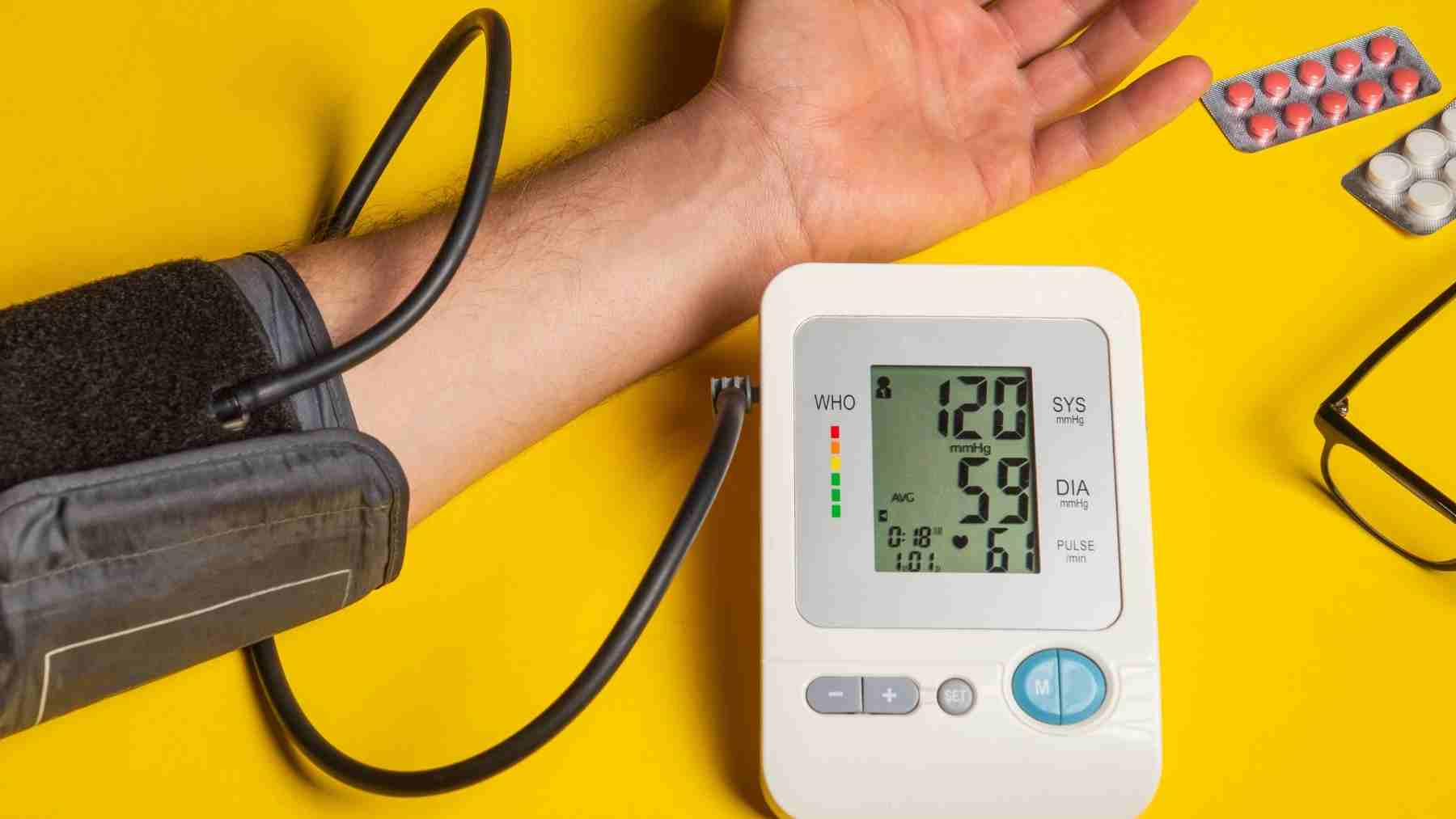
The two numbers on a blood pressure reading are not just random figures on a screen. The top number reflects pressure when the heart beats, and the bottom number reflects pressure when it rests between beats. A quiet cuff reading can reveal a lot.
Blood flow and arteries
The key idea is the endothelium, the thin inner lining of blood vessels. It sounds like a simple wrapper, but it behaves more like a tiny control center. It helps vessels relax, keeps blood moving smoothly, and calms inflammation.
In healthy conditions, blood often moves in a smooth pattern called laminar flow. Picture cars moving steadily in lanes during light traffic. It is organized, quiet, and efficient.
But changes in vessel stiffness, vessel size, plaque buildup, or small injuries can make flow more chaotic. That rougher movement can scrape against the inner lining again and again. The damage may be tiny each time, but repeated damage is what makes it matter.
Why the cycle feeds itself
When the endothelium is injured, vessels may tighten more easily and inflammation can rise. Think of a garden hose with a slightly stiff wall and a narrower opening. The same water can still move through, but it needs more push.
That is why hypertension is often described as a disease of the microvasculature, meaning the network of very small blood vessels. These small channels are not dramatic, and no one talks about them at dinner. Still, they help decide how hard the whole system has to work.
The kidney also joins the loop. If it senses that blood flow is too low, it can activate a hormone system that tells the body to tighten vessels and hold on to salt and water. In practical terms, that means more fluid in circulation and more pressure in the pipes.
Risk factors still count
None of this removes responsibility from prevention. It makes prevention feel less like blame and more like maintenance. You are not just “being good” when you stop smoking or walk after dinner; you are lowering the strain on a sensitive system.
U.S. federal heart research guidance lists age, family history, lifestyle habits, medicines, and other medical conditions as risk factors. It also notes that some medicines, including certain antidepressants, decongestants, hormonal birth control pills, aspirin, and ibuprofen, can make blood pressure harder to control.
Sleep apnea, chronic kidney disease, obesity, and poor-quality sleep can also raise risk. So can long-running stress, the kind that keeps the body on alert even after the workday ends. That does not mean stress alone explains hypertension, but it can add weight to the system.
What patients can take away
The first takeaway is simple. Measuring blood pressure is not a one-time chore for older adults; it is a basic health signal, like checking the weather before leaving home. Since hypertension often has no symptoms, feeling fine is not proof that everything is fine.
Another practical detail is measuring both arms. Montes de Oca warned that a difference of more than 15 points between arms should raise concern about possible vascular disease. It is not a diagnosis on its own, but it is a clue worth discussing with a clinician.
The bigger message is that hypertension care should combine habits, medication when needed, and a search for hidden drivers. That can include kidney disease, sleep apnea, medication side effects, and resistant cases that do not respond as expected. At the end of the day, controlling pressure is not just about pushing one number down; it is about protecting the vessels that keep every organ supplied.
The main official health information cited in this article has been published by the World Health Organization, MedlinePlus, and the National Heart, Lung, and Blood Institute.