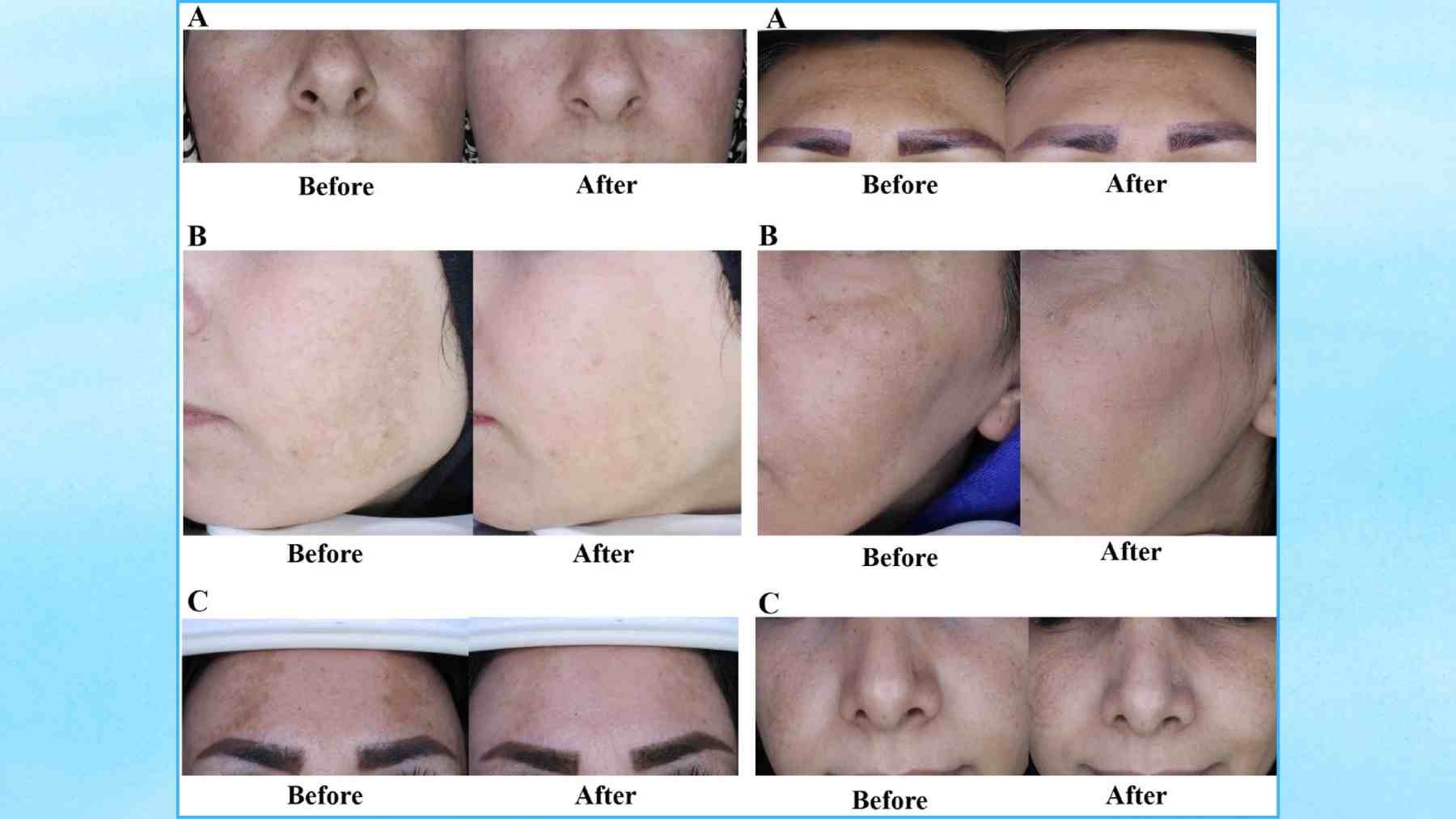
If you’ve ever looked in the mirror and wondered why those brown or gray-brown patches on your cheeks or upper lip keep coming back, you’re not alone. Melasma is common, stubborn, and for many people, emotionally exhausting.
Now, a new randomized, double-blind clinical trial suggests there may be safer ways to treat it without leaning so heavily on hydroquinone. The headline finding is simple. Two tranexamic acid plus niacinamide creams performed about as well as hydroquinone for improving melasma over three months, with fewer serious side effects.
What the researchers actually tested
The trial enrolled 99 adults with melasma and split them into three groups, each using a different topical cream for three months. One group used a “niosomal” tranexamic acid 2% plus niacinamide 2% cream, another used a conventional tranexamic acid 5% plus niacinamide 4% cream, and a third used hydroquinone 4%.
Dermatologists tracked changes using objective measures like melanin index and the modified Melasma Area and Severity Index (mMASI). Patients also reported quality-of-life changes, which matters more than people sometimes admit when the issue is on your face and shows up in every selfie.
Hydroquinone still works, but the tradeoff can be rough
Hydroquinone has long been treated as the go-to topical option for melasma, mostly because it can reduce pigment by interfering with melanin production. For many patients, it does help. That’s why it’s still widely used.
But this trial adds to a familiar complaint. Hydroquinone was linked to more frequent and more intense reactions, including severe burning, redness, hypersensitivity reactions, and even ochronosis in some cases. And if you’ve ever tried to stick with a product that stings every night, you already know how quickly motivation disappears. That discomfort can also push people toward harsh “fixes,” which is where irritation spirals. If you’re dealing with persistent irritation, it’s usually a sign your routine needs a reset, not more active ingredients piled on top.
Why tranexamic acid plus niacinamide is getting attention
Tranexamic acid and niacinamide target pigmentation through different pathways, which is part of the appeal. Niacinamide is a form of vitamin B3 that can help reduce pigment transfer within the skin, while tranexamic acid has been studied for melasma because it may interrupt signaling that contributes to excess melanin production.
In this trial, both tranexamic acid plus niacinamide formulations led to meaningful reductions in melasma severity measures over time, similar to hydroquinone. The key difference was tolerability. Serious adverse reactions were far less common in the tranexamic acid plus niacinamide groups.
What “niosomal” delivery means in real life
The niosomal cream used lower concentrations of the active ingredients yet still performed similarly to the higher-dose conventional version. That matters because it hints at a practical advantage. If delivery systems can improve how a product penetrates and stays in the skin, you may not need as much of the active drug to get results.
For everyday use, that could translate into fewer side effects and a better chance of sticking with treatment long enough to see results. At the end of the day, consistency is the quiet factor that decides whether a plan works or fizzles out after week two.
Sunscreen is not optional, even when you’re “just running errands”
Melasma is strongly linked to ultraviolet exposure, and any topical treatment is fighting an uphill battle if the skin keeps getting hit with UV day after day. The study participants were instructed to use sunscreen with SPF 30 or higher repeatedly throughout daylight hours, which fits what most dermatologists emphasize in real-world care.
It’s also the easiest part to underestimate. People remember sunscreen at the beach, but forget it on the drive to work, walking the dog, or sitting by a sunny window. And once pigment pathways are reactivated, you can end up chasing the same spots again and again.
UV exposure is also tied to broader skin aging processes, including collagen breakdown, which is why researchers keep circling back to prevention. Some newer reporting in our cosmetics coverage has even explored signals that may influence collagen production and cellular energy, though that’s a different lane than melasma treatment itself. Still, the message overlaps. Protecting skin early is easier than repairing it later.
The mental health impact is real, and the data backs it up
Melasma is often treated like a purely cosmetic concern, but the psychological burden can be significant. The Scientific Reports paper itself points to evidence connecting melasma with depression and anxiety, which makes sense if you’ve ever felt your confidence dip because of visible facial patches.
A separate systematic review and meta-analysis has reported higher depression rates in people with melasma compared with controls. That doesn’t mean melasma “causes” depression in every case, but it does reinforce why treatment conversations should include quality of life, not just pigment scores.
If you notice symptoms like persistent worry, rumination, or feeling “on edge” about how you look in public, it can help to name what’s happening. Some psychology writers point out that the “high alert” feeling many people carry can mask anxiety in ways that are easy to miss. Others argue that stress around an uncertain future can intensify when you feel you have little control, including over your own skin.
What to ask your dermatologist before switching products
This study does not mean everyone should throw out hydroquinone tomorrow. It does suggest that tranexamic acid plus niacinamide creams can be reasonable alternatives to discuss, especially if you’ve had side effects or relapse issues.
It also highlights a basic but important point. Melasma is chronic and relapsing for many people, and management often works best as a long game. That means sunscreen habits, gentle routines, and realistic expectations, plus working with a dermatologist who can tailor treatment to your skin type, triggers, and tolerance.
The study was published on Scientific Reports.