Why are so many people suddenly talking about magnesium malate as if it were a one-stop answer for low energy, stress, and weak bones? The short version is that magnesium itself is essential for hundreds of processes in the body, including energy production, muscle function, nerve signaling, and bone health. But when you look closely, the science behind magnesium malate is more nuanced than the sales pitch.
In practical terms, magnesium malate is a supplement form that combines magnesium with malic acid. That sounds impressive, and it may help some people who are not getting enough magnesium in the first place. Still, the strongest evidence supports magnesium’s general role in the body, not the idea that magnesium malate is a proven fix for anxiety, depression, and exhaustion all at once.
What magnesium malate actually is
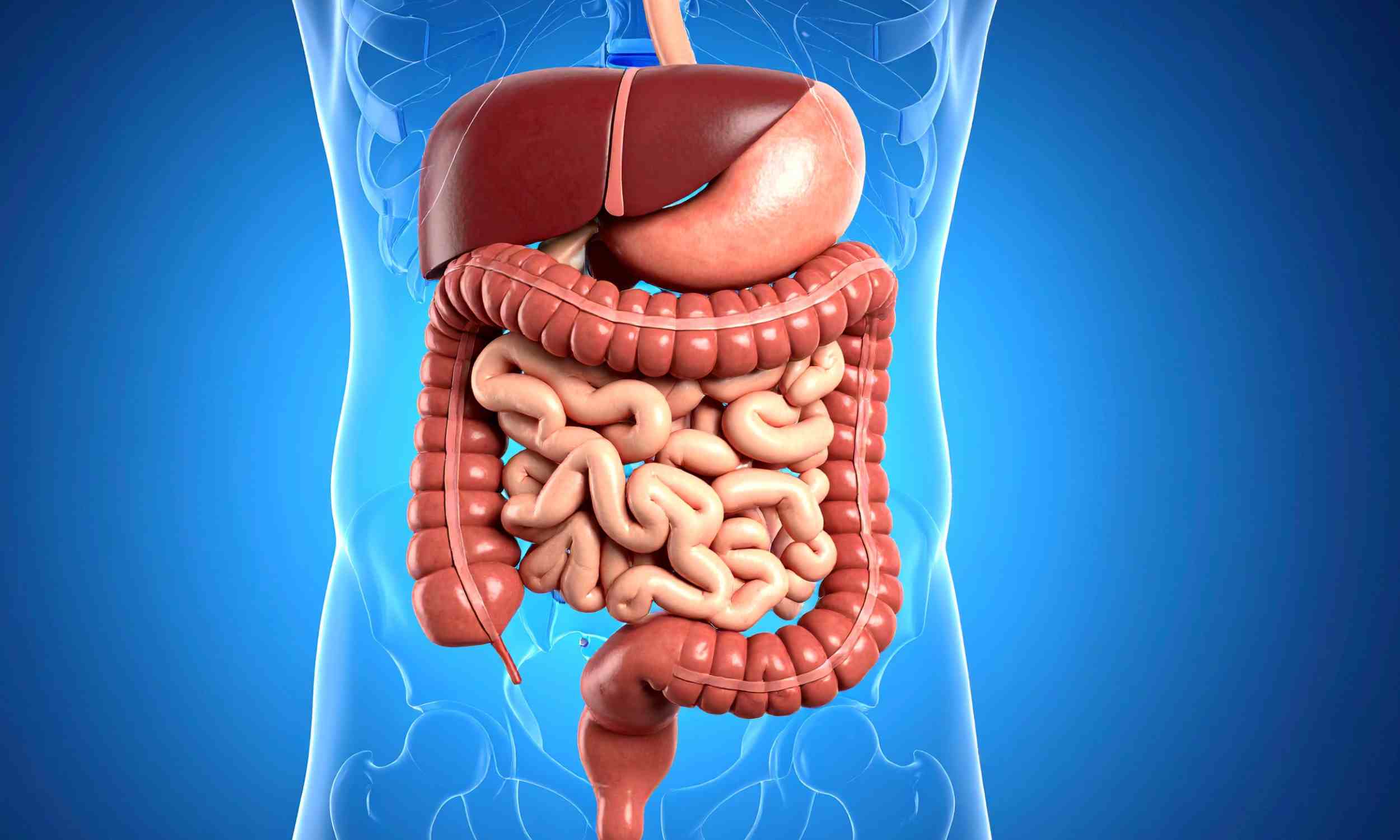
Magnesium is a mineral your body needs every day, and the National Institutes of Health says it acts in more than 300 biochemical reactions. It helps convert food into energy, supports muscles and nerves, and plays a direct part in keeping bones strong. About half to 60% of the body’s magnesium is stored in bone, which gives you a sense of how central it is.
Magnesium malate is simply one supplement form among many. The NIH Office of Dietary Supplements notes that absorption differs across supplement types and highlights some forms, such as citrate and chloride, as better absorbed than oxide, but it does not present magnesium malate as the clearly established winner. That matters because many bold claims online go further than the evidence does.
Why it may help with fatigue
If your magnesium intake is low, feeling drained can be part of the picture. MedlinePlus and the NIH both list fatigue and weakness among the early signs of magnesium deficiency, alongside nausea, poor appetite, and muscle problems. In other words, for some people, that worn-out feeling may have less to do with motivation and more to do with nutrition.
That does not mean everyone with tiredness needs a supplement. What the evidence shows, for the most part, is that magnesium helps the body make and use energy normally, so bringing levels back up may help if someone is running low. It is a reasonable angle, but it is not the same thing as saying magnesium malate will boost energy in every healthy person who buys a bottle.
The anxiety and depression question
This is where the story gets more careful. A 2024 systematic review published in Cureus found supplemental magnesium is likely useful for mild anxiety and insomnia, especially in people who start out with low magnesium status, while a 2023 meta-analysis of randomized trials found depression results were still inconsistent even though some benefit appeared in the data.
There is also a notable randomized clinical trial led by Elizabeth Tarleton at the University of Vermont and published in PLOS ONE. That study reported improvement in adults with mild to moderate depression after magnesium supplementation, but it tested magnesium chloride, not magnesium malate, and it does not prove one supplement form is a mental health cure. That is an important distinction.
What the evidence says about bones and muscles
Bone health is one of the more solid parts of the magnesium story. The NIH says magnesium contributes to bone structure, affects the cells that build and break down bone, and is linked in population studies to better bone mineral density. It also helps regulate vitamin D and hormones involved in bone balance, which is why low magnesium can be a concern over time.
Muscles matter here too. Magnesium helps with muscle contraction and relaxation, and low levels can show up as cramps, weakness, or spasms. So yes, people who exercise often, older adults, and people with poor diets may notice a difference when low intake is corrected. But the bigger takeaway is still about correcting a gap, not chasing a miracle product.
Where the magnesium malate hype runs ahead of science
If magnesium malate is often marketed for fibromyalgia, chronic fatigue, and mood symptoms, does the research back that up? Not strongly. A review in Medwave led by Isadora Ferreira concluded that the combination of magnesium and malic acid made little or no difference for pain or depressive symptoms in fibromyalgia, based on the limited trial evidence available.
That does not make the supplement useless. It just means the best-supported claim is the simplest one. Magnesium matters, many Americans do not get enough magnesium, and some people may benefit from supplements when diet falls short or deficiency is suspected. The NIH estimates that 48% of Americans get less magnesium from food and drinks than they need, which helps explain why this mineral keeps coming up in health conversations.
Who should be cautious
More is not always better. The NIH says high doses of magnesium from supplements can cause diarrhea, nausea, and cramping, and very large amounts can become dangerous, especially for people with kidney problems. The tolerable upper level from supplements for adults is 350 mg per day unless a clinician advises otherwise.
At the end of the day, what this supplement is trying to do is fill a real nutritional need. For someone eating plenty of leafy greens, beans, nuts, seeds, and whole grains, the payoff may be limited. For someone with low intake, fatigue, cramps, or a medically confirmed deficiency, it may be more relevant, though ongoing anxiety, depression, or bone loss still deserve proper medical care and not just another item in the supplement aisle.
The main official source discussed here was published on the U.S. Department of Health and Human Services site.