Could one of the most common vitamins on the shelf help calm a disease that can dominate daily life? New research suggests vitamin D may do more than support bones. In people with inflammatory bowel disease, a 12-week course of weekly supplements was linked to lower inflammation and a more balanced immune response to gut bacteria.
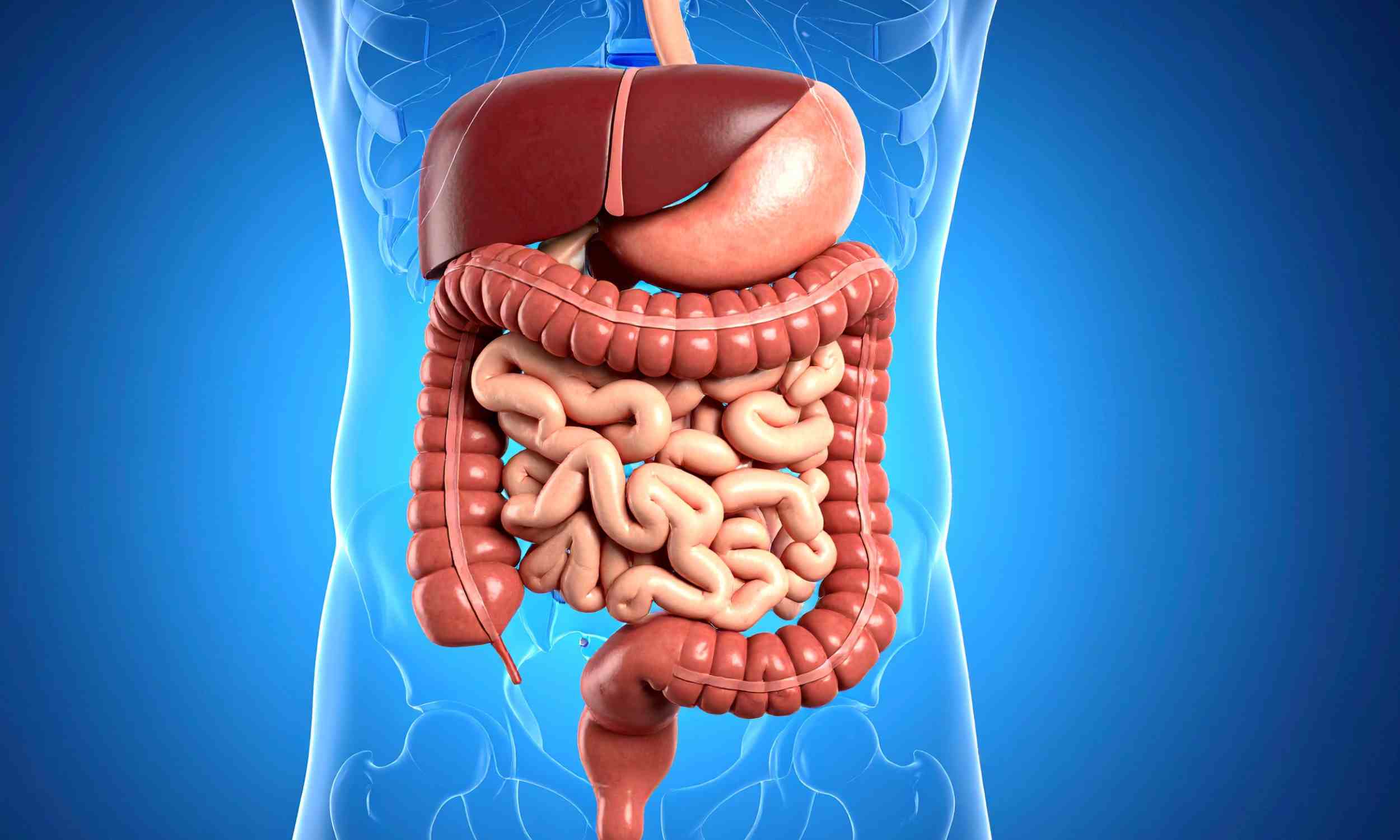
That matters because inflammatory bowel disease, or IBD, often means abdominal pain, diarrhea, bleeding, fatigue, and flare-ups that can make school, work, or even a short trip feel harder than it should. The catch is important. Researchers say the study was small and not randomized, so patients should not change vitamin D use on their own.
Why it matters
Crohn’s disease and ulcerative colitis are the two main forms of IBD. In both, the immune system reacts abnormally and fuels long-term inflammation in the digestive tract. Scientists think part of the problem is a breakdown in “immune tolerance,” which is the body’s ability to live peacefully with the harmless bacteria that normally belong in the gut.
That idea is a big deal because most current treatments are built to turn inflammation down after it is already burning. This study points to something slightly different. It suggests vitamin D may help the body respond to the gut microbiome in a steadier and more protective way.
How the study worked
The work was led by John Mark Gubatan, a gastroenterologist at Mayo Clinic in Florida. His team followed 48 adults with Crohn’s disease or ulcerative colitis who started the study with low vitamin D levels, then gave them weekly vitamin D supplements for 12 weeks while collecting blood and stool samples before and after treatment.
The researchers were not only asking whether patients felt better. They also used advanced lab tools to track how antibodies, immune cells, and gut bacteria were interacting. In simple terms, they were looking for signs that vitamin D could change the conversation between the immune system and the microbes it meets every day.
What changed in the gut
After treatment, levels of immunoglobulin A, also called IgA, went up, while immunoglobulin G, or IgG, went down. IgA is an antibody that helps defend the gut lining without causing as much inflammatory damage, while IgG is more often linked to aggressive immune reactions in this setting. The team also saw shifts in immune signaling and in regulatory cells that help keep inflammation under control.
That does not sound flashy, but it may be the biggest takeaway. Rather than simply dampening inflammation, vitamin D appeared to push the immune system toward better tolerance of normal gut bacteria. In other words, the body may have become a little less likely to treat familiar microbes like enemies.
The clinical signs
The immune changes were not happening only on paper. Researchers also reported better disease activity scores and lower fecal calprotectin, a stool marker doctors use to track intestinal inflammation. Lower calprotectin does not equal a cure, but it can be a useful sign that the gut is quieter than before.
For patients who keep cycling through flares, that kind of shift matters. It could mean fewer days built around symptoms and fewer moments when every plan depends on where the nearest bathroom is. Even so, the study does not show that vitamin D can replace standard drugs. At most, it suggests the vitamin could become part of a more personalized treatment strategy after larger trials.
Why doctors are still cautious
The lead author was clear about the limits, saying, “We saw encouraging signals, but this was not a randomized trial.” In practical terms, that means the findings are promising but not final, because the study did not include the kind of comparison needed to show cause and effect with confidence. The work also received support from the National Institutes of Health, although that does not change the need for stronger evidence.
This result also did not appear out of nowhere. Earlier research has linked low vitamin D levels with worse outcomes in IBD, including a higher risk of ulcerative colitis relapse during remission, and a 2018 study reported lower fecal calprotectin after vitamin D replacement in some patients with active ulcerative colitis. At the same time, previous clinical studies have not always produced clear or consistent answers, which is why experts still want larger controlled trials.
What patients should take from it
The main takeaway is not that everyone with Crohn’s disease or ulcerative colitis should rush to buy supplements. Vitamin D is easy to find, but the researchers warned that dosing needs to be individualized, especially in people living with chronic inflammation. Their advice was simple, saying patients should “work with their healthcare team.”
At the end of the day, this study matters because it points to a more precise way of thinking about gut disease. Instead of only trying to smother inflammation after it starts, doctors may one day help the immune system relearn how to tolerate the bacteria that belong in the intestines. That is still a work in progress, but it is a meaningful one.
The main study has been published in Cell Reports Medicine.