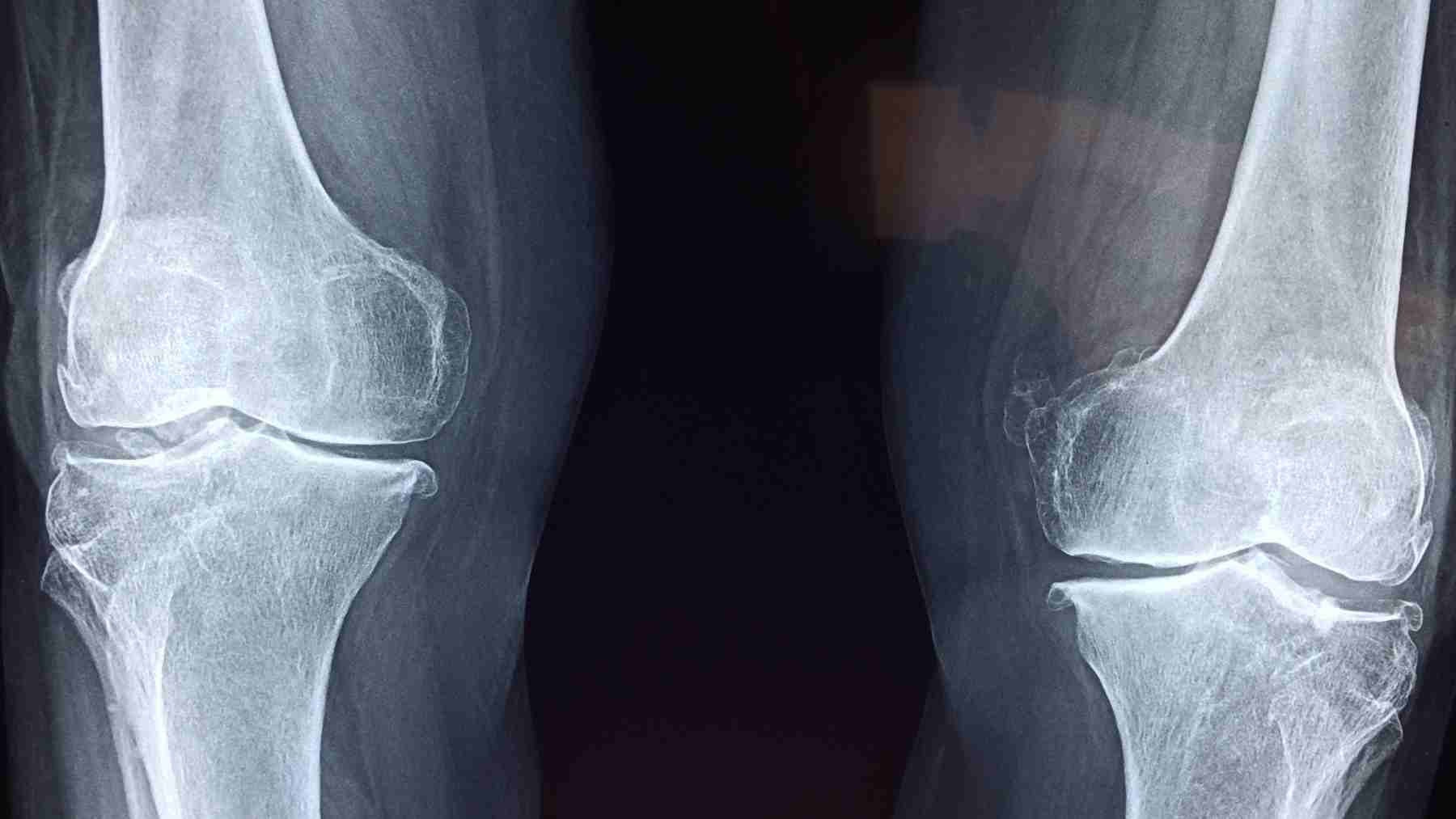
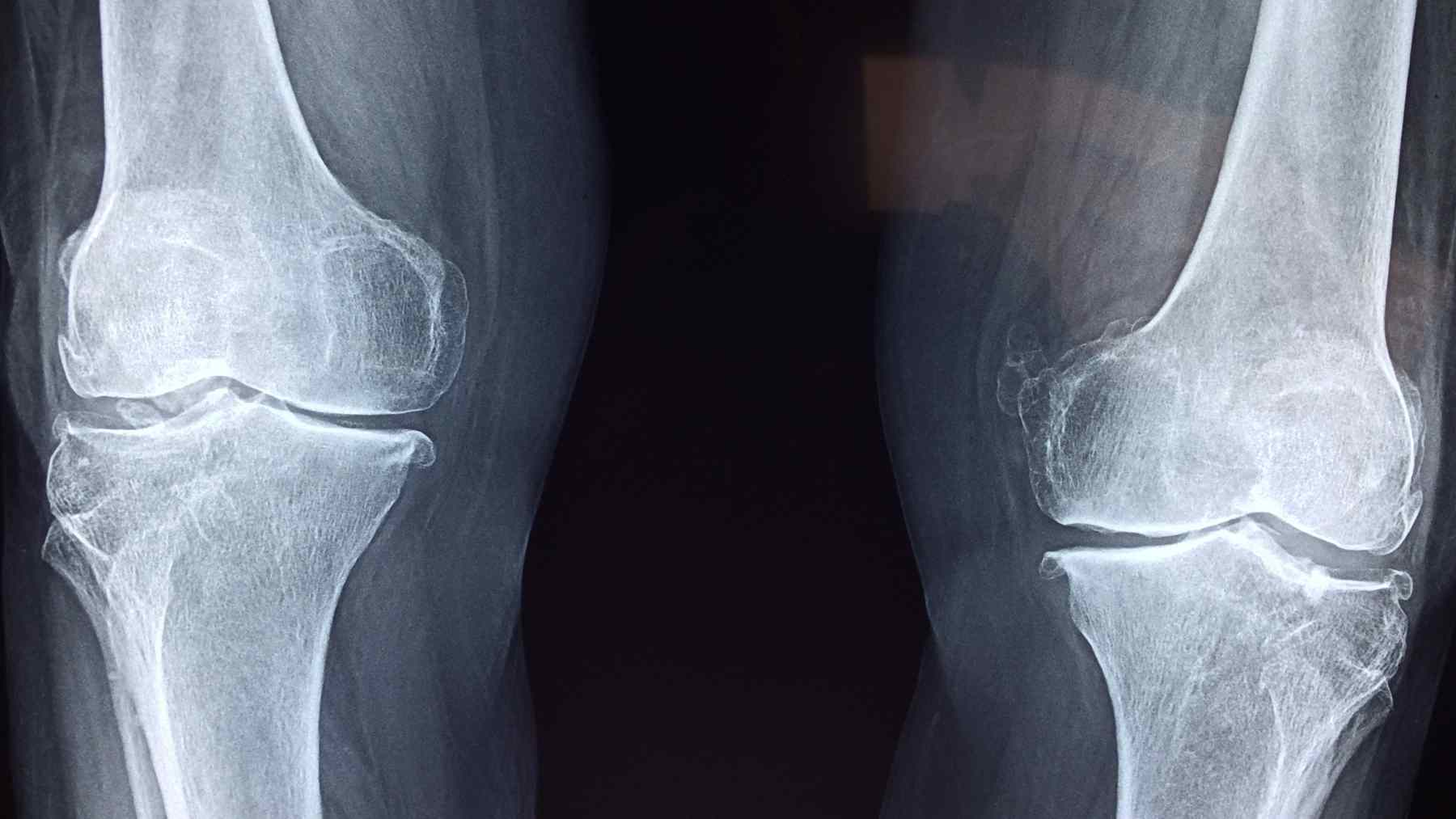
Osteoporosis can turn an ordinary slip into a broken wrist, a cracked vertebra, or a hip fracture that changes daily life overnight. In a paper published June 30, 2025, researchers found that activating a little-studied cell receptor called GPR133 boosted bone strength and eased osteoporosis-like bone loss in mice, pointing to a potential new drug target.
So what makes this receptor different from other leads that come and go? GPR133 appears to act like a messenger for the physical forces bones feel during everyday movement, then translates those forces into “build more bone” signals inside cells.
It is still early research, but it hints at a future where treatment could copy the body’s own mechanical cues instead of only slowing bone breakdown.
Why osteoporosis often shows up too late
The National Institute of Arthritis and Musculoskeletal and Skin Diseases calls osteoporosis a “silent disease” because many people have no clear symptoms until a bone breaks. Some notice back pain from a spine fracture or a slow loss of height, but those clues can show up late.
In the United States, the Bone Health and Osteoporosis Foundation estimates about 10 million people have osteoporosis, and another 44 million have low bone density that raises fracture risk. That helps explain why doctors focus so much on fall prevention, from loose rugs to dark stairwells to that patch of ice you did not see.
Germany faces a similar burden. The International Osteoporosis Foundation reports about 5.6 million people with osteoporosis in Germany and more than 831,000 fragility fractures, breaks that can happen from a fall at standing height, each year, or roughly 95 every hour.
Bones are living tissue, not fixed scaffolding
Even though bones feel rock-solid, they are constantly being renewed through a process called remodeling. Osteoclasts remove old bone, then osteoblasts build new bone in its place, with other bone cells helping coordinate that cycle.
This activity shifts depending on whether bones are “loaded” by movement or “unloaded” by inactivity. When the cleanup side stays too active for too long, the body can lose more bone than it replaces.
A receptor called GPR133 gets scientists’ attention
A receptor is a kind of switch on a cell’s surface, picking up outside cues and triggering internal responses. Scientists at Leipzig University say GPR133, also called ADGRD1, responds to mechanical strain and to contact between neighboring bone cells, signals bones experience during normal movement.
When it switches on, it supports osteoblasts and restrains osteoclasts, tipping the balance toward stronger bone. Researchers are also interested because GPR133 belongs to the large family of G protein-coupled receptors, or GPCRs, which are already a mainstay of modern medicine.
A large analysis counted 516 approved drugs that target GPCRs, around 36 percent of all approved drugs, showing how often these “cell switches” can be turned into therapies. That track record makes a newly understood receptor like GPR133 especially tempting as a drug target.
What AP503 did in mouse models of bone loss
To test whether GPR133 really matters for bone strength, the scientists studied mice with genetic changes that impair the receptor. Those animals showed early signs of reduced bone density, a pattern that resembles osteoporosis in humans.
Next came AP503, a compound identified through a computer-assisted screening approach designed to find chemicals that can stimulate GPR133. Professor Ines Liebscher, the study’s lead investigator at the Rudolf Schönheimer Institute of Biochemistry within the Faculty of Medicine, said “we were able to significantly increase bone strength in both healthy and osteoporotic mice.”
The improvement also showed up in a mouse model meant to mimic postmenopausal bone loss, a common pathway into osteoporosis. That matters because osteoporosis is often called a silent disease, and many people do not know they have it until a fracture occurs.
Bone and muscle losses often travel together
For many older adults, the bigger problem is not just brittle bones, it is the combination of weaker bones, weaker muscles, and less stable balance. In earlier animal research, activating GPR133 with AP503 was also linked to improved skeletal muscle strength, suggesting a possible two-in-one approach to frailty.
That matters because the fall that causes a fracture often starts with muscle weakness. Lead author Dr Juliane Lehmann pointed to that overlap, saying the parallel strengthening of bone “once again highlights the great potential this receptor holds for medical applications.”
If bone and muscle could be supported together, it might help address falls and fractures that rise as populations age. It is an appealing direction, but it raises practical questions about safety, dosing, and long-term effects.
What has to happen before any human treatment
The most important limitation is simple. The strongest evidence still comes from mice, and mouse bones are not identical to human bones.
Researchers will need studies that look at human cells and tissues, then carefully designed clinical trials that test safety and effectiveness in people. Current care includes medicines that slow bone loss and, for some patients, medicines aimed at rebuilding bone, but treatment decisions can be complicated.
The US Food and Drug Administration notes that osteoporosis medicines can have side effects and should be chosen with a healthcare professional rather than started or stopped casually. For now, AP503 is a promising lab result, not something you will see at a pharmacy.
The main study has been published in Signal Transduction and Targeted Therapy.